
NICU sims be certain labor and shipping and delivery crew is expertly well prepared for complicated deliveries.
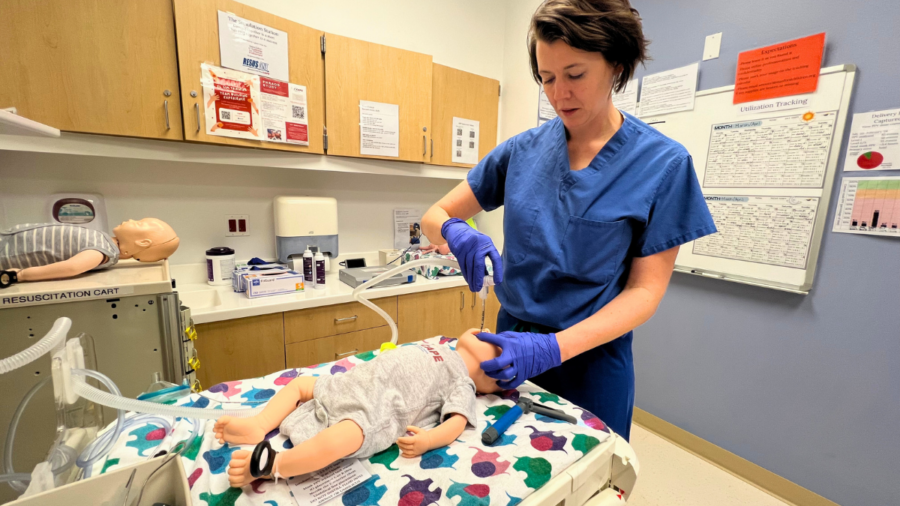
In the essential 1st moments of lifestyle, the neonatal labor and supply care team’s readiness can mean the big difference concerning daily life and demise. At Lucile Packard Children’s Hospital Stanford, an ground breaking simulation program makes sure that this crew is organized for just about anything.
Recently, more than 40 employees users took element in an open household for the NICU Simulation Station, which was formulated by Audrey Moore, a board-qualified neonatal nurse practitioner (NNP), NNP guide of the Resus Just one Resuscitation Basic safety and General performance Improvement Method, and designer of the NICU Simulation Station at Packard Children’s Healthcare facility. ”Simulation allows participants to acquire or enhance their information, expertise, and team efficiency in anticipation for crucial situations in the shipping area,” Moore states.
The NICU Simulation Station, funded by a grant from the Association of Auxiliaries for Young children, is one of a kind in that it makes it possible for teams to observe specialized skills prior to all deliveries and just-in-time training prior to elaborate deliveries.
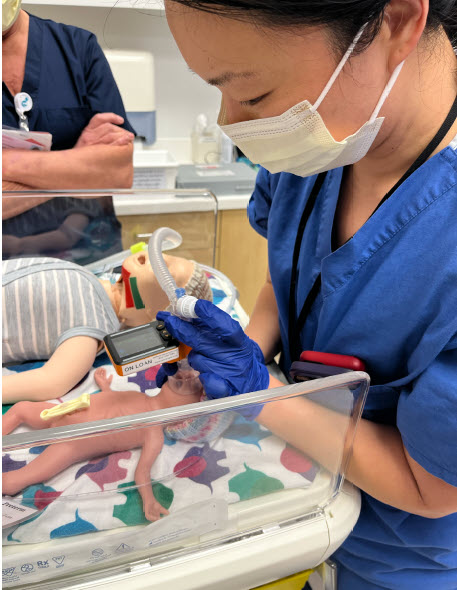
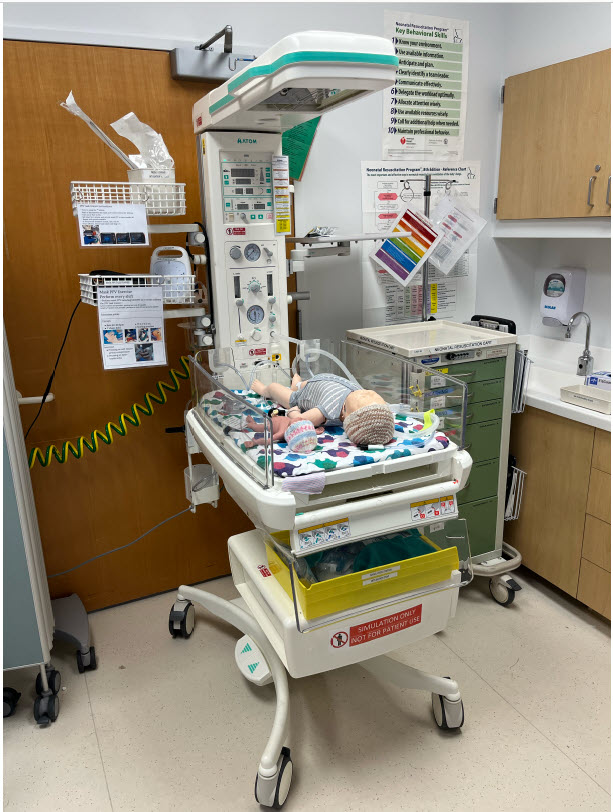
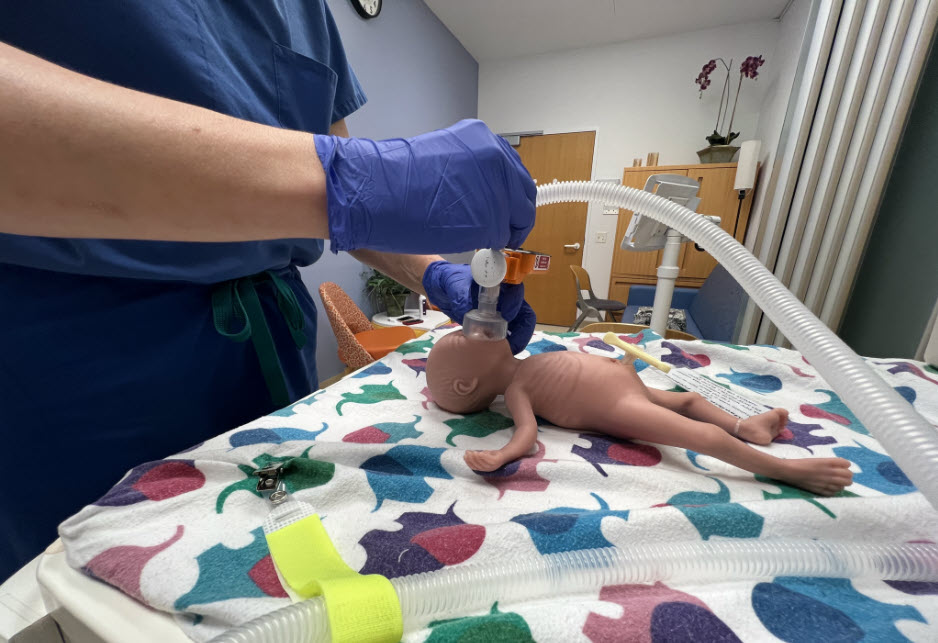
Started in 2018, the Resus 1 Software was designed by neonatologists at Packard Children’s Medical center to enhance patient safety by examining staff effectiveness in the supply space. With the addition of the NICU Simulation Station, all of the health and fitness treatment pros concerned in the care of newborns at the time of beginning (neonatal nurse practitioners, NICU nurses, respiratory therapists, neonatology hospitalists, neonatologists and trainees, these as inhabitants and fellows in these disciplines) now receive critically vital schooling on a every day foundation.
Just-in-time instruction and briefing is now finished to prepare for each routine and complicated shipping and delivery place cases, permitting teams to put together for sufferers this sort of as those born at the limitations of viability (hardly halfway through a 40-7 days pregnancy) and whole-term neonates with congenital malformations that complicate their resuscitation and stabilization. In each individual circumstance, it’s essential for the neonatology crew to act quickly and efficiently to provide the client with the very best chance for an optimal final result.
In just the initial two months of procedure, many neonatology teams participated in 28 pre-shipping and delivery briefings and just-in-time education sessions. In addition, wellness care pros experienced extra than 100 possibilities to apply life-preserving interventions this kind of as optimistic pressure ventilation and intubation.
“Given the many distinct mixtures of individuals who arrive together to go to a elaborate shipping and delivery at any certain stage in time, using the simulation station for briefings, observe of technological skills, just-in-time teaching, and larger sized scale simulations ensures that each and every team member can conduct at a significant amount when a newborn’s everyday living is at danger,” Moore, states.
Lou Halamek, MD, Professor of Pediatrics, Director of Neonatal Resuscitation and founder of both the Resus One Program and the Heart for Sophisticated Pediatric and Perinatal Education and learning (CAPE) at Packard Children’s Hospital, is effusive in his praise for what Moore has achieved with the assistance of the Resus A single group, which involves Nicole Yamada, MD, Professional medical Director – Neonatal Crucial Treatment Transportation Staff, and Janene Fuerch, MD. Clinical Director – Neonatal ECMO Director.
“Audrey Moore has worked unbelievably challenging to provide this Simulation Station to everybody in the NICU,” states Dr. Halamek. “It is an vital ingredient of Resus 1 and the CAPE Circle of Safety, wherever serious-world human efficiency info drives our instruction attempts. Her vision, perseverance and tenacity have created a tool that will actually assistance preserve newborn lives.”






